Discovering Dysautonomia, a disease that affects more than 70 million people in the world
A Professional Insight from Dr. Joel Sanchez, Dysautonomia Expert in Puerto Vallarta
Dysautonomia, also known as autonomic dysfunction, is a broad term that refers to a group of medical conditions which are caused by a dysfunction of the autonomic nervous system (ANS). The autonomic nervous system is responsible for regulating involuntary body functions, such as heart rate, blood pressure, digestion, temperature, and more. However, when the ANS doesn’t function properly, it can lead to a wide range of symptoms and problems in multiple organ systems.
In this post, we will explore this complex condition that affects more than 70 million people worldwide. Moreover, we’ll discover how Dr. Joel Sanchez, a leading Dysautonomia expert in Puerto Vallarta, has become a source of hope for those facing this medical challenge.
Dysautonomia Symptoms
Dysautonomia symptoms can include heart palpitations, fatigue, weakness, gastrointestinal problems, difficulty regulating body temperature, and more. Nonetheless, because dysautonomia encompasses a wide range of conditions with different causes, treatment options can vary. Thus, management may involve medications to control symptoms, lifestyle changes, physical therapy, and in some cases, addressing the underlying cause if one is identified.
If you suspect you have dysautonomia or are experiencing symptoms related to autonomic nervous system dysfunction, it’s important to consult a healthcare professional for proper diagnosis and a treatment plan tailored to your specific condition.
Factors that may contribute to the development of dysautonomia
In many cases, the exact cause of dysautonomia is unknown. Nevertheless, there are several factors that have been linked to an increased risk of developing this condition. For example, some of the risk factors and possible triggers include:
- Genetics: In some cases, dysautonomia has a genetic component. Therefore, certain types of dysautonomia, like Familial Dysautonomia (FD) or hereditary forms of POTS, can be inherited. Also, if a family member has dysautonomia, other family members may have a higher risk of developing this condition.
- Autoimmune Disorders: Some autoimmune diseases, such as Sjögren’s syndrome, or lupus, can affect the autonomic nervous system, leading to dysautonomia.
- Infections: Certain infections, such as Lyme disease, have been associated with the development of dysautonomia.
- Neurological Conditions: Neurological disorders like Parkinson’s disease, multiple system atrophy (MSA), or certain neuropathies can lead to dysautonomia as part of their clinical manifestation.
- Trauma or Injury: In some cases, physical trauma or injury, such as a spinal cord injury, can damage nerves or disrupt autonomic function, leading to dysautonomia symptoms.
- Chronic Stress: Prolonged periods of chronic stress or psychological trauma can potentially impact autonomic nervous system function.
Nonetheless, it’s important to note that dysautonomia can manifest in different ways, and the specific contributing factors can vary widely. Consequently, diagnosis and management should be performed by healthcare professionals such as cardiologists or interventional cardiologists. Fortunately, these specialists can evaluate a patient’s medical history, conduct appropriate tests, and recommend a treatment plan tailored to one’s specific condition. Treatment may involve addressing underlying causes, managing symptoms, and making lifestyle modifications to improve overall quality of life.
Diagnostic tests and disease management
Dysautonomia is a difficult disease to diagnose due to the variety of symptoms it may present. Thus, early and accurate detection is essential to provide appropriate treatment, management and support. To achieve this goal, Dr. Joel Sanchez uses the following specialized tests and procedures to identify this complex disease:
- Detailed medical history: Dr. Sanchez begins the diagnostic process by conducting a thorough interview with his patients. This helps him to know the symptoms, medical history, and risk factors of his patients.
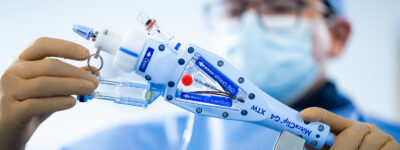
- Tilt Test: This test, performed at our CMQ Riviera Nayarit Hospital, measures the nervous system’s response to changes in posture. In this case, our specialist observes how the patient’s heart and blood pressure react when moving from a horizontal to a vertical position.
- Monitoring Blood Pressure: Our cardiologist uses this technique to register blood pressure over a prolonged period of time. Through this method, he can identify abnormal changes that could be indicative of dysautonomia.
- Imaging Studies: In some cases, our specialist may request imaging studies such as an MRI scan, to rule out other underlying conditions.
Tilt Test at CMQ Riviera Nayarit Hospital
When it comes to diagnosing and addressing conditions such as dysautonomia, it is essential to have the right equipment and expertise. At Hospital CMQ Riviera Nayarit, our tilt table test performs key diagnostic studies for the diagnosis of nervous system disorders.
The tilt test consists of evaluating the response of the nervous system to postural changes. During this test, the patient lies on his or her back on a special table that is gradually tilted at different angles. While this occurs, our team will monitor the patient’s heart rate and blood pressure. This test lasts approximately 45 to 90 minutes.
Benefits of the Tilt Test study
The benefits of the Tilt Test are significant. For example, one of the most prominent benefits is that it provides an accurate diagnosis of conditions related to heart rate and blood pressure. In addition, once an autonomic disorder has been diagnosed, the Tilt Test provides valuable information for designing a personalized treatment plan. This may include lifestyle modifications, dietary changes, medications, or other targeted therapies to address symptoms and improve the patient’s quality of life.
The Tilt Test is just one of the many medical resources available at Hospital CMQ Riviera Nayarit to assist in the diagnosis and treatment of disorders such as Dysautonomia. Our commitment to quality medical care allows us to provide our patients the most specialized tests and services to serve their needs. If you or a loved one has unexplained symptoms related to dysautonomia, we are here to help.
What are the types of dysautonomia?
There are several different types of dysautonomia, and the specific symptoms and underlying causes can vary widely. Some common types and conditions associated with dysautonomia include:
Postural Orthostatic Tachycardia Syndrome (POTS)
POTS is characterized by an abnormal increase in heart rate when a person changes position, typically when transitioning from lying down to standing up. This can lead to symptoms such as dizziness, lightheadedness, and fainting.
Neurocardiogenic Syncope (NCS)
NCS is a condition where changes in position or other triggers cause a sudden drop in blood pressure and fainting.
Multiple System Atrophy (MSA)
MSA is a progressive neurodegenerative disorder that affects the autonomic nervous system and can lead to problems with movement, balance, and autonomic functions.
Pure Autonomic Failure (PAF)
PAF involves a gradual loss of autonomic function and can result in symptoms such as orthostatic hypotension (low blood pressure when standing) and difficulty regulating body temperature.
Familial Dysautonomia (FD)
FD is a rare genetic disorder that primarily affects people of Ashkenazi Jewish descent. It causes a range of symptoms related to autonomic dysfunction, including difficulty swallowing and respiratory issues.
Autonomic Neuropathy
This condition can result from various underlying causes, such as diabetes, autoimmune diseases, or alcoholism. It leads to damage to the nerves that control autonomic functions.
Dysautonomia and stress; is there a direct link between the two?
Indeed, there is a relationship between dysautonomia and stress. According to our specialists, stress can influence the severity of symptoms and the quality of life of people with dysautonomia. The reason for this is that stress can affect the function of the autonomic nervous system. Therefore, when stress is added to existing nervous system dysfunction, symptoms such as tachycardia, dizziness, and fatigue can worsen.
For this reason, our cardiologists recommend stress management techniques such as relaxation, meditation, physical exercise, and physical therapy. In this case, it is important for those suffering from dysautonomia to be supported by a multifunctional team of healthcare professionals. This will help to develop strategies and obtain the necessary treatment to address both the physical and emotional aspects of dysautonomia.
Find your Dysautonomia expert in Puerto Vallarta
Dr. Joel Sanchez, with his experience and dedication in the field of interventional cardiology, has earned a special place in the medical community of Puerto Vallarta. His patient-centered approach and profound knowledge of Dysautonomia have made a significant difference in the lives of those who struggle with this disease. Book your appointment now!
Frequently asked questions about dysautonomia
Dysautonomia is a broad term that refers to a group of medical conditions characterized by dysfunction of the autonomic nervous system (ANS). This system controls many automatic things in our bodies. Things we don’t even think about, like heart rate, blood pressure, digestion, and sweating. Normally, these things happen without us having to tell our bodies what to do. But with dysautonomia, this system doesn’t work quite right. It can make you feel lightheaded, dizzy, have heart palpitations, or even faint when you stand up. It can mess with your digestion, making you feel sick or have stomach problems. It can also affect your body’s ability to control your temperature.
Symptoms of dysautonomia can vary widely. Some of the most common symptoms include:
- Dizziness or feeling faint when standing up
- Unusually rapid heartbeat
- Chronic fatigue
- Gastrointestinal problems and nausea
- Problems with body temperature regulation
- Sweating and cold skin
- Blurred vision
- Muscle weakness
- Difficulty concentrating
Treatment of dysautonomia usually involves several specialists, as it can affect multiple areas of the body. Most often, specialists who are well prepared to diagnose and treat dysautonomia include a multidisciplinary team of clinical cardiologists, interventional cardiologists, gastroenterologists, endocrinologists, and neurologists.
Dysautonomia can be caused by various factors, and the exact cause often depends on the specific type or form of dysautonomia. Some causes might be linked to genetics, autoimmune diseases, infections, neurological disorders, and chronic stress, among others. However, in many cases, the exact cause of dysautonomia remains unknown, and it may be considered idiopathic, meaning that doctors can’t pinpoint a specific cause.
Dysautonomia itself is not an autoimmune disease. It is a group of conditions characterized by dysfunction of the autonomic nervous system (ANS), which controls involuntary bodily functions. Sometimes, dysautonomia can occur as a symptom of certain autoimmune diseases, but it is not classified as an autoimmune disease on its own.
The diagnosis of dysautonomia typically involves a combination of medical history evaluation, clinical assessment, and specialized tests. It is essential to consult with a healthcare professional, often a cardiologist or a neurologist, to determine the specific type of dysautonomia and its underlying cause.
The outcome of dysautonomia varies depending on the specific type, underlying cause, and individual factors. In some cases, dysautonomia may improve or stabilize with treatment and lifestyle modifications. However, for many people, dysautonomia is a chronic condition that may require ongoing management to control symptoms and improve quality of life.